
-
 Written By:
Alex Herrera
Written By:
Alex Herrera
-
 Edited By:
Christina Holmes
Edited By:
Christina Holmes
-
 Clinically Reviewed By:
Dr. Ash Bhatt, MD, MRO
Clinically Reviewed By:
Dr. Ash Bhatt, MD, MRO
Fentanyl vs. Heroin: Why Synthetic Opioids Pose a Greater Risk Today
The opioid epidemic that began reshaping American communities in the late 1990s looked very different from the one unfolding today. Where heroin once defined the most acute end of opioid misuse, a synthetic compound, smaller in volume and nearly invisible to the naked eye, has rewritten the risk calculus entirely.
Fentanyl is now the leading driver of overdose deaths in the United States, and New Jersey has not been spared. For families, first responders, and anyone navigating a relationship with opioids, their own or someone they love, understanding the difference between fentanyl and heroin is now a matter of life and death.
This article is a clear, clinically grounded account of how these two substances compare, why fentanyl has made the current crisis so much more lethal, and what expert-led treatment at Legacy Healing NJ looks like for those ready to find a way out.
Key Takeaways
|
Heroin: A Powerful but Traditional Opioid
Heroin is derived from morphine, itself extracted from the opium poppy plant. It has been classified as a Schedule I controlled substance in the United States since 1970, meaning it has no accepted medical use and carries a high potential for abuse. For much of the late twentieth century, heroin was the opioid of greatest clinical concern in addiction medicine.
When heroin enters the bloodstream, it crosses the blood-brain barrier and converts back to morphine, binding rapidly to opioid receptors throughout the brain and central nervous system. The result is an intense wave of euphoria, followed by a prolonged sedated state. Pain signals are suppressed. Anxiety dissolves. For someone in emotional or physical pain, the relief can feel profound, and that relief is precisely what makes it so dangerous.
Tolerance develops quickly. The dose that produced euphoria last week no longer delivers it this week. The dose required escalates, and with it, the physical dependence. Withdrawal from heroin, the nausea, cramping, insomnia, and severe psychological distress that follow when use stops, is one of the most physically punishing experiences in addiction medicine. It is also one of the primary reasons people cannot simply stop on their own.
“Heroin rewires the brain’s reward system. What begins as a choice to use becomes, over time, a physiological need, the body insisting on what the brain has learned to require.”
New Jersey has a long, documented history with heroin. Its geography, a dense transportation corridor between New York and Philadelphia, has historically made it a distribution hub, and communities across the state have carried the consequences of that proximity for decades. But even against that backdrop, the emergence of fentanyl has introduced a threat of a different order entirely.
Fentanyl: The Rise of Synthetic Opioids
Fentanyl is a fully synthetic opioid, meaning it is manufactured in a laboratory rather than derived from any plant-based source. It was developed in 1960 and has legitimate, carefully controlled medical applications: it is used in hospital settings for the management of severe acute pain, during surgical procedures, and in transdermal patches for patients with advanced cancer or chronic pain conditions who require continuous opioid therapy.
In those clinical contexts, fentanyl is administered in precisely measured, medically supervised doses. The margin for error is understood and managed. The problem arises, catastrophically, when fentanyl enters the illicit drug supply.
Over the past decade, illicitly manufactured fentanyl (IMF) has flooded drug markets across the United States at a scale that has overwhelmed public health infrastructure. Unlike heroin, which requires poppy cultivation and a relatively labor-intensive extraction process, fentanyl can be synthesized in clandestine laboratories using precursor chemicals, many of which have been sourced from overseas. The result is a product that is cheaper to produce, easier to transport in smaller quantities, and far more profitable per unit than heroin.
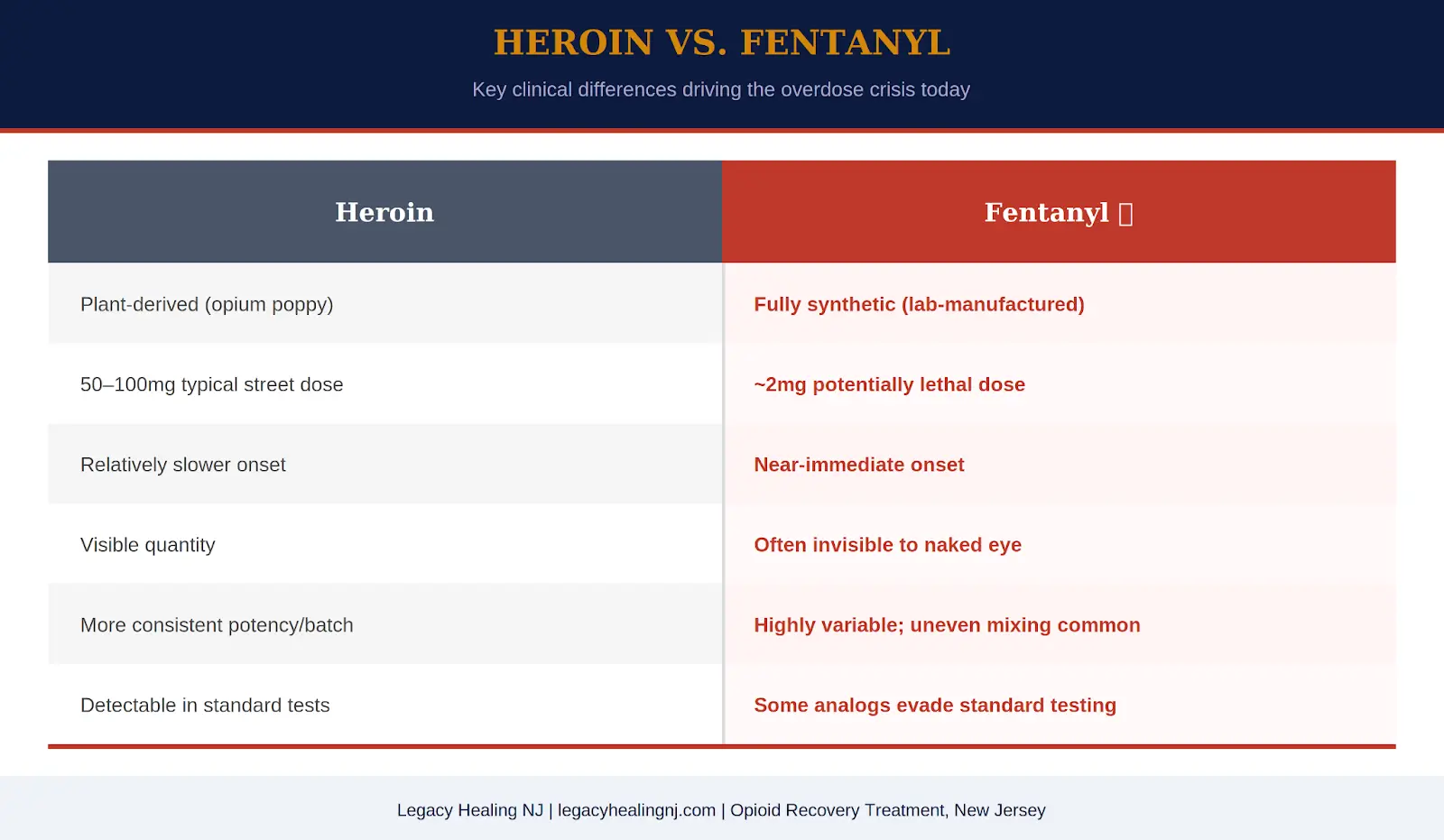
| Key distinction: Heroin is plant-derived. Fentanyl is entirely lab-manufactured.
This difference has profound implications for supply chains, potency consistency, and overdose risk. Illicitly manufactured fentanyl (IMF) is now the dominant form found in the U.S. drug supply. |
The rise of illicit fentanyl has been documented across every demographic. It is no longer primarily a concern for people already using heroin or other opioids. Fentanyl has been found in cocaine, methamphetamine, counterfeit prescription pills, and MDMA, substances whose users may have no opioid tolerance whatsoever, making a first exposure potentially fatal.
Potency Differences That Make Fentanyl Uniquely Lethal
The clinical comparison between heroin and fentanyl in terms of potency is a matter of category. Fentanyl is estimated to be approximately 100 times more potent than morphine and 50 times more potent than heroin by weight. Its analog carfentanil, which has appeared in the illicit supply, is estimated to be 10,000 times more potent than morphine.
What this means in practical terms is sobering. A lethal dose of fentanyl is measured in micrograms, millionths of a gram. Two milligrams is considered a potentially lethal dose for a person with no opioid tolerance. That quantity is invisible to the naked eye. It cannot be measured without laboratory equipment. It cannot be detected by sight, smell, or taste.

The margin between a dose that produces the desired effect and a dose that stops breathing is extraordinarily narrow with fentanyl, far narrower than with heroin. In heroin, that margin, while still dangerous, allowed for some degree of error. With fentanyl, there is effectively no margin. A miscalculation of milligrams, a slightly uneven mix in a counterfeit pill, an inconsistent cut in a batch of powder, can be the difference between a high and a fatal overdose.
Tolerance also complicates the picture in both directions. People who have been using opioids long-term may require higher doses to achieve the same effect, but if they stop using and then relapse after a period of abstinence, their tolerance has reset. Returning to a previously “normal” dose of a fentanyl-containing substance after a break is one of the most common scenarios leading to fatal overdose.
From Dr. Ash Bhatt
“What people need to understand is that fentanyl has effectively removed the margin for error. In clinical terms, we’re no longer talking about a substance where dose can be estimated safely. Even a microscopic variation can determine whether someone experiences a high or a fatal overdose. That level of unpredictability is what makes fentanyl fundamentally different from heroin.”
The Hidden Danger: When Fentanyl Is in Drugs You Don’t Expect
One of the most alarming developments of the current opioid crisis is that people who have no idea it is present.
Illicit fentanyl is now routinely found in the drug supply far beyond the opioid category. It has been detected in counterfeit pills pressed to look exactly like legitimate prescription medications, Xanax bars, OxyContin tablets, Adderall capsules. It has been found in cocaine and methamphetamine. It has been found in MDMA sold at music festivals.
| ⚠ Critical Safety Warning
Fentanyl cannot be seen, smelled, or tasted in a drug mixture. Fentanyl test strips can detect its presence, but are not available everywhere. Naloxone (Narcan) can reverse a fentanyl overdose, but time is critical. In New Jersey, naloxone is available without a prescription at most pharmacies. If you suspect an overdose: call 911 immediately, administer naloxone if available, place the person on their side. |
The mechanism behind this contamination is partly economic and partly logistical. Fentanyl is so potent that even small quantities add significant effect to a larger batch of a less potent drug. For drug traffickers, adulterating a supply with fentanyl increases perceived potency and reduces the quantity of the primary drug needed, improving margins while creating enormous, often invisible, risk to the end user.
For someone who has never used opioids, or who uses stimulants with no opioid tolerance, encountering fentanyl unexpectedly can be fatal within minutes. The respiratory depression that fentanyl produces is rapid and severe. There may be no time to recognize what is happening, no time to call for help, no time for intervention.
From Dr. Ash Bhatt
“One of the most dangerous shifts we’re seeing is that fentanyl exposure is no longer limited to opioid users. I’ve treated individuals who had no intention of using opioids but were exposed through contaminated substances. The reality today is that any illicit drug use carries a fentanyl risk, and in many cases, people don’t realize it until it’s too late.”
How Synthetic Opioids Are Reshaping the Addiction Crisis in New Jersey
The introduction of illicit fentanyl into the drug supply has done more than increase overdose risk, it has structurally changed the addiction crisis itself. The economic and logistical advantages fentanyl offers to drug trafficking organizations have accelerated its displacement of heroin as the dominant opioid in street markets. In many parts of New Jersey, heroin is no longer reliably available without fentanyl contamination, and in some markets, what is sold as heroin is fentanyl entirely.
The consequences are visible in the data. New Jersey has consistently ranked among the states with the highest opioid overdose death rates in the country. Fentanyl and fentanyl analogs now account for the overwhelming majority of those deaths. The demographic profile of overdose victims has also shifted: the crisis is no longer concentrated in any single community, age group, or income level. It reaches professionals, students, parents, and first responders.
| New Jersey Opioid Crisis: Key Context
NJ has one of the highest opioid overdose death rates in the nation. Fentanyl and its analogs account for the vast majority of opioid fatalities statewide. More than 6 in 10 counterfeit pills seized nationally contain a potentially lethal fentanyl dose (DEA). First responders in NJ now routinely carry naloxone, but rapid professional treatment remains essential. |
For families watching a loved one struggle with opioid dependence, the urgency of intervention has never been greater. The window between active addiction and a fatal overdose is narrower now than it has ever been. This is not alarmism, it is the clinical and epidemiological reality that shapes how Legacy Healing NJ approaches opioid treatment: with urgency, without judgment, and with the full weight of evidence-based medicine behind every decision.
From Dr. Ash Bhatt
“Fentanyl hasn’t just increased overdose risk—it has fundamentally changed the nature of the crisis. The timeline from active use to a fatal outcome is much shorter now, and the populations affected are far broader. This is why, from a clinical standpoint, we approach every case with urgency. Delaying treatment today carries far greater risk than it did even a few years ago.”
Recognizing Opioid Dependence: What to Look For
One of the most common barriers to treatment is the belief that the problem is not serious enough to warrant it. Opioid use disorder rarely announces itself clearly. It develops gradually, often behind a convincing facade of normal functioning.
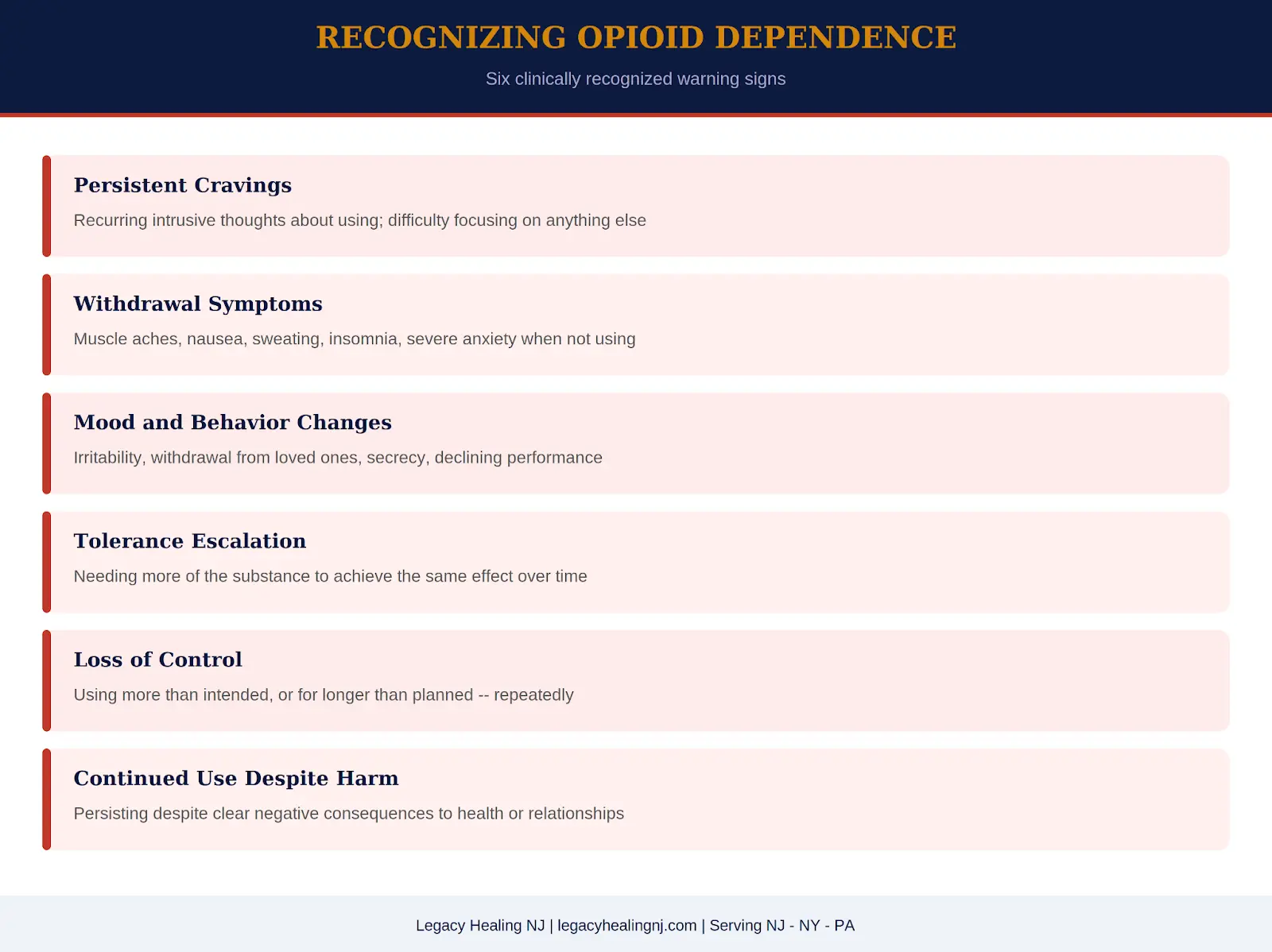
The following indicators are clinically recognized signs that opioid dependence may have developed, regardless of whether the substance is heroin, fentanyl, or a prescription opioid.
Persistent Cravings
Cravings for opioids, intrusive, recurring thoughts about using, difficulty concentrating on anything else, a sense that relief is only possible with the substance, are a hallmark of opioid use disorder. When cravings begin to organize around acquisition and use, the relationship with the substance has crossed from physical dependence into the territory of addiction.
Withdrawal Symptoms
Physical withdrawal from opioids, including muscle aches, sweating, nausea, vomiting, insomnia, severe anxiety, and dysphoria, begins within hours to days of the last dose and can last for several weeks in acute form. Post-acute withdrawal, a more prolonged period of mood instability, sleep disruption, and low-grade discomfort, can persist for months. The severity of withdrawal is one of the primary reasons people cannot stop opioids without medical support.
Changes in Mood and Behavior
Unexplained mood swings, increased irritability, social withdrawal, declining performance at work or school, loss of interest in previously meaningful relationships and activities, secrecy around finances or whereabouts, these behavioral shifts are frequently the first signs that family members notice. They are neurobiological consequences of sustained opioid use that disrupt the brain’s normal emotional regulation systems.
If you recognize these signs, in yourself or someone close to you, it is not a moment for shame or judgment. It is a moment for action. Opioid use disorder is a treatable medical condition, and early intervention significantly improves outcomes.
Professional Treatment for Opioid Recovery at Legacy Healing NJ
The stakes of opioid addiction in the fentanyl era are too high for anything less than comprehensive, medically supervised care. Self-managed withdrawal from opioids is not only deeply uncomfortable, it is clinically risky, and the rate of relapse without professional support is high. Legacy Healing NJ was built to change that equation.
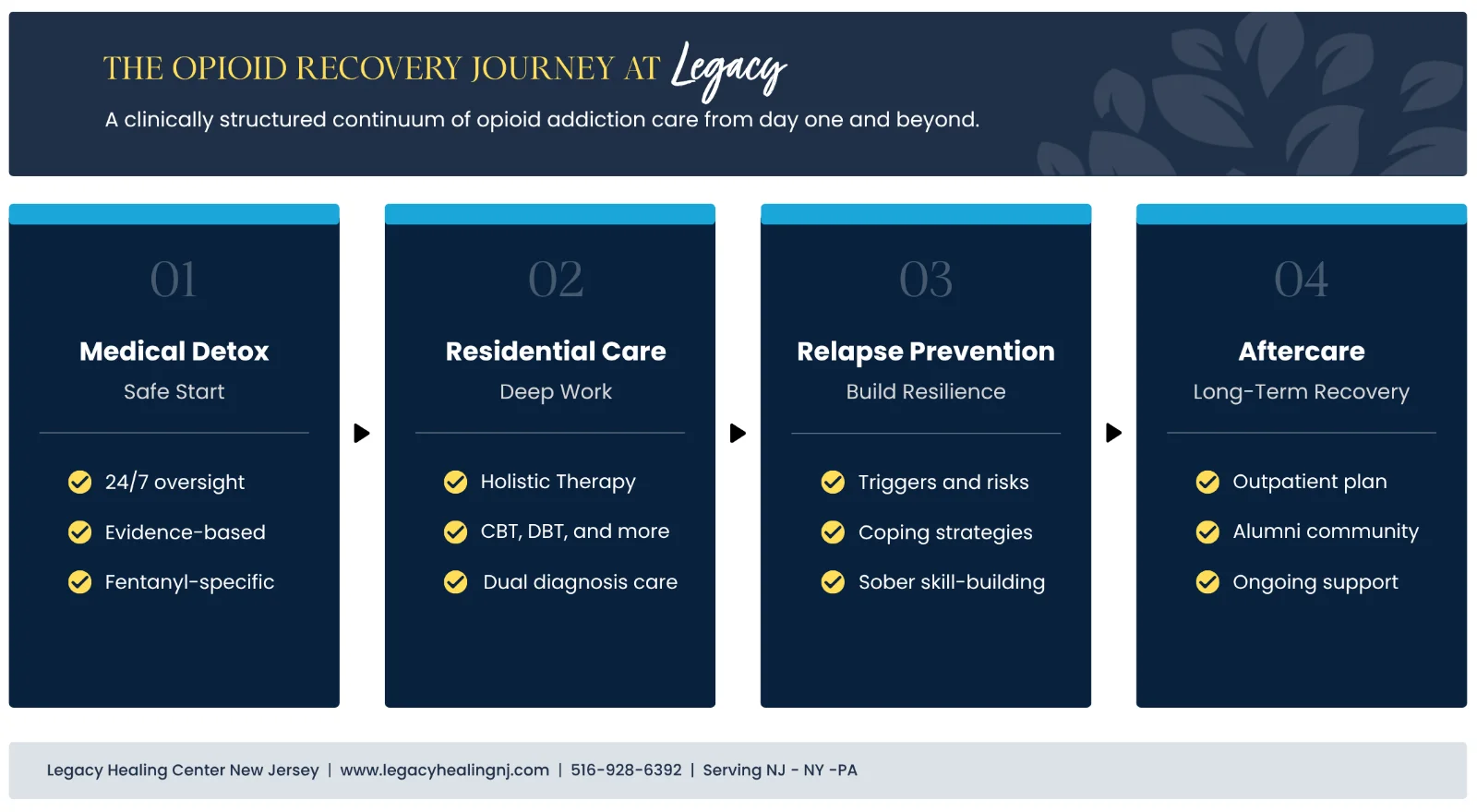
Our approach to opioid recovery is grounded in evidence, individualized to each person, and structured to address every dimension of the condition, the physical dependency, the psychological drivers, the behavioral patterns, and the life circumstances that will shape long-term recovery.

Medical Detox: Where Safe Recovery Begins
The first step in opioid recovery is medically supervised detoxification. At Legacy Healing NJ, our board-certified physicians oversee every aspect of the withdrawal process, monitoring vitals, managing withdrawal symptoms with evidence-based medications including buprenorphine and methadone where clinically appropriate, and ensuring that the detox process is as safe and as comfortable as possible.
For fentanyl specifically, detox requires particular clinical attention. Fentanyl has a longer duration of action in certain formulations, and withdrawal timelines can differ from heroin. Our clinical team accounts for these distinctions in every individual treatment plan.
Evidence-Based Therapy and Relapse Prevention
Detox addresses the physical dependency. Therapy addresses everything else. Legacy Healing NJ’s therapeutic programming includes Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), Motivational Enhancement Therapy, and trauma-focused modalities for clients whose substance use is rooted in unprocessed trauma, which, in our clinical experience, describes a significant proportion of those seeking opioid treatment.
Relapse prevention is woven into every stage of treatment, not addressed as a standalone module at the end of a program, but integrated from the first day of residential care through every phase of the recovery continuum. Understanding personal triggers, building coping strategies, and developing the self-awareness to recognize early warning signs of relapse are skills we work on systematically with every client.
A Supportive, Luxury Environment for Healing
Recovery requires more than the right medications and the right therapy. It requires an environment that supports it, one where the daily experience of being in treatment does not itself feel like a punishment. Legacy Healing facilities in New Jersey offer the privacy, comfort, and clinical excellence that allow our clients to focus entirely on their recovery.
We serve residents of New Jersey, New York, and Pennsylvania, and we understand that many of our clients arrive carrying the weight of years of struggle, complicated family dynamics, and in many cases, profound shame. Our clinical environment is designed to make that weight feel lighter, not by minimizing the seriousness of the work, but by doing it in a space where every person is treated with dignity, competence, and genuine care.
“The bravest thing a person in active addiction can do is ask for help. Our job is to make certain that when they do, the help waiting for them is worth the courage it took to ask.”
Hope Beyond Opioid Addiction
The fentanyl crisis has made the conversation about opioid addiction more urgent. Every day, people who have been in the grip of opioid dependence for years find their way to lasting recovery with the right support. The prognosis is not determined by how long someone has struggled. What it is determined by: the quality of the treatment, the comprehensiveness of the support, and the willingness of the person in front of us to do the difficult, courageous work of healing.
Legacy Healing NJ is here for every part of that process, from the first conversation to the long years of recovery that follow.
If you or someone you love is struggling with fentanyl, heroin, or any opioid, today is not too late. And the right help is closer than you may think.
“Addiction is not the end of your story. It is the chapter before the one where everything changes.”
Expert Insights from Dr. Ash Bhatt
Questions & Answers Fentanyl Vs Heroin Risk Comparison
How does fentanyl change the overdose risk compared to heroin in real-world cases?
How does fentanyl change the overdose risk compared to heroin in real-world cases?
Fentanyl dramatically increases overdose risk because of how little is needed to suppress breathing. With heroin, there is already risk, but fentanyl narrows the margin of safety to the point where even a trace amount can be fatal. What makes it more concerning is that many individuals don’t even realize they are consuming it.
Why is fentanyl so much more dangerous than heroin?
Why is fentanyl so much more dangerous than heroin?
Several factors combine to make fentanyl uniquely lethal: its extreme potency means a dose too small to see with the naked eye can be fatal; its presence in counterfeit pills and non-opioid drugs means users may encounter it without knowing; illicit manufacturing results in uneven mixing and inconsistent potency within a single batch; and its rapid onset leaves little time for intervention when an overdose occurs.
Why are people overdosing even when they think they are not using opioids?
Why are people overdosing even when they think they are not using opioids?
I’ve treated many cases where patients believed they were using substances like cocaine or counterfeit prescription pills. The reality is that fentanyl is now widely mixed into these drugs. This hidden exposure is one of the biggest reasons we’re seeing a sharp rise in unexpected overdoses, even among those without a history of opioid use.
Is there any way to tell if a drug contains fentanyl before using it?
Is there any way to tell if a drug contains fentanyl before using it?
Unfortunately, in most cases, there is no reliable way to detect fentanyl without test strips. From a medical standpoint, I advise patients and families to assume that any illicit substance could be contaminated. The unpredictability of the current drug supply is what makes fentanyl particularly dangerous.
Does naloxone work the same way for fentanyl as it does for heroin?
Does naloxone work the same way for fentanyl as it does for heroin?
Naloxone can absolutely save lives in both cases, but with fentanyl, I often see the need for multiple doses. Its potency and rapid onset can make reversal more challenging. That’s why immediate medical attention is critical, even if naloxone has been administered.
What makes fentanyl addiction more complex to treat than heroin addiction?
What makes fentanyl addiction more complex to treat than heroin addiction?
From a treatment perspective, fentanyl dependence can develop more quickly and may involve more intense withdrawal symptoms. It also requires careful medical management during detox. We tailor treatment plans specifically to address these complexities, ensuring both safety and long-term recovery support.
What should someone do immediately if they suspect fentanyl exposure or overdose?
What should someone do immediately if they suspect fentanyl exposure or overdose?
The most important step is to call emergency services right away. In my practice, I emphasize that time is critical. Administer naloxone if available, but do not wait to see if it works, professional medical care is essential to stabilize the individual and prevent fatal outcomes.
Disclaimer: This content is not a diagnosis or medical advice, it is provided for educational purposes only. If you or a loved one is struggling with substance use, please consult a qualified medical professional.

Dr. Ash Bhatt MD. MRO
Quintuple board-certified physician and certified medical review officer (AAMRO) with 15+ years of experience treating addiction and mental health conditions. Read More…
Table of Contents
Most Insurance Policies
Cover Treatment.
Find out what treatment programs you qualify for in less than 2 minutes.
"*" indicates required fields
Ready to Get Help?
One call can change everything. Our experienced admissions team is here to guide you to the right treatment. All calls are 100% confidential.





