
-
 Written By:
Todd Ludwig
Written By:
Todd Ludwig
-
 Edited By:
Christina Holmes
Edited By:
Christina Holmes
-
 Clinically Reviewed By:
Dr. Ash Bhatt, MD, MRO
Clinically Reviewed By:
Dr. Ash Bhatt, MD, MRO
What Is High-Acuity Care and How Does It Support Complex Mental Health Recovery?
Key Takeaways
- High-acuity mental health care is designed for complex, treatment-resistant conditions that require more than weekly outpatient therapy, offering intensive clinical oversight, structured support, and flexible treatment pacing.
- Not all mental health challenges respond to standard care, especially when trauma, emotional dysregulation, co-occurring disorders, or repeated treatment failures are involved, high-acuity programs are built specifically for these layered needs.
- Effective high-acuity treatment follows a phase-based approach, prioritizing safety and stabilization first, then trauma processing, and finally reconnection and functional recovery, rather than rushing individuals through care.
- Progress is measured by real-life functioning and emotional regulation, not just symptom reduction, focusing on stability, coping skills, and the ability to manage daily life over time.
If you’re reading this, there’s a good chance you or someone you love has been struggling with mental health challenges that haven’t gotten better despite treatment. Perhaps you’ve been told your condition is “treatment-resistant” or “complex,” and you’re wondering what that really means and where to go from here.
You’re not alone, and you haven’t failed. What you’re experiencing is more common than most people realize. Approximately 30% of individuals with depression don’t respond adequately to standard treatments. This is where high-acuity mental health care comes in, offering intensive support designed for people whose needs go beyond what traditional outpatient therapy can address.
This guide will help you understand what high-acuity care really means, how it works, and what steps to take if you think you might need this level of support.
What Does “High-Acuity” Really Mean in Healthcare?
In healthcare, “acuity” measures how severe and urgent someone’s condition is. Think of it as a spectrum: a sprained ankle might be low-acuity, while a heart attack is high-acuity (it requires immediate, specialized intervention). The same concept applies to mental health care.
High-acuity mental health conditions involve severe symptoms that create immediate safety concerns. These situations demand more than weekly therapy sessions; they require intensive, structured care with continuous clinical oversight.
It involves multiple therapy sessions per week, psychiatric oversight, 24/7 clinical support, and often a residential or day program format where you can focus solely on recovery without the demands of work, school, or home responsibilities. For those seeking comprehensive mental health treatment, understanding these intensity levels helps determine the right approach.
Who Is Considered a High-Acuity Patient?
High acuity simply means your situation requires a different level of support. Complex patient profiles often include several intersecting challenges that compound each other.
Consider whether any of these situations describes your experience:
- You’ve tried at least two different medications or therapy approaches without significant improvement
- You experience frequent suicidal thoughts or have engaged in self-harm behaviors
- Your symptoms make it difficult or impossible to work, attend school, or maintain relationships
- You’re dealing with both mental health and substance use challenges simultaneously
- You’ve been hospitalized for psychiatric reasons more than once
- You experience severe mood swings, panic attacks, or dissociative episodes that disrupt daily life
- You have a history of complex trauma that hasn’t been adequately addressed in previous treatment
Programs offering residential treatment are specifically designed to address these complex presentations.
What Makes Mental Health Cases High-Intensity?
Understanding psychiatric complexity helps explain why some mental health challenges require more intensive intervention and there are several factors that makes mental health cases high intensity, such as:
1. When Emotions Feel Uncontrollable
Emotional dysregulation is a hallmark of high-intensity cases. This means experiencing emotions so intensely that they lead to impulsive or dangerous behaviors. You might go from feeling fine to being in crisis within minutes, struggle to calm down once upset, or find that typical coping strategies simply don’t work.
2. Due to Trauma and it’s Complication
If you experienced chronic abuse, neglect, or violence, especially during childhood, your mental health needs are likely more complex than standard depression or anxiety. These cases require trauma-informed approaches that prioritize safety and gradual processing. This is why specialized trauma therapy programs use phase-oriented approaches, moving at your pace rather than pushing you to confront painful experiences before you’re ready.
3. In Case of Treatment Resistance
Treatment resistance doesn’t mean nothing will help. It means the standard first-line approaches aren’t sufficient for your particular situation. You may need specialized medication combinations, brain stimulation therapies like TMS, intensive psychotherapy, or treatment for co-occurring conditions that have been maintaining the depression. High-acuity programs have the resources and expertise to explore these advanced treatment options.
How Is Therapy Adapted for Complex High-Intensity Clients?
High-acuity treatment uses adaptive techniques and therapist-paced protocols in a structured approach, designed to prevent re-traumatization. It’s a three-phase model that ensures you develop stability before processing traumatic memories.
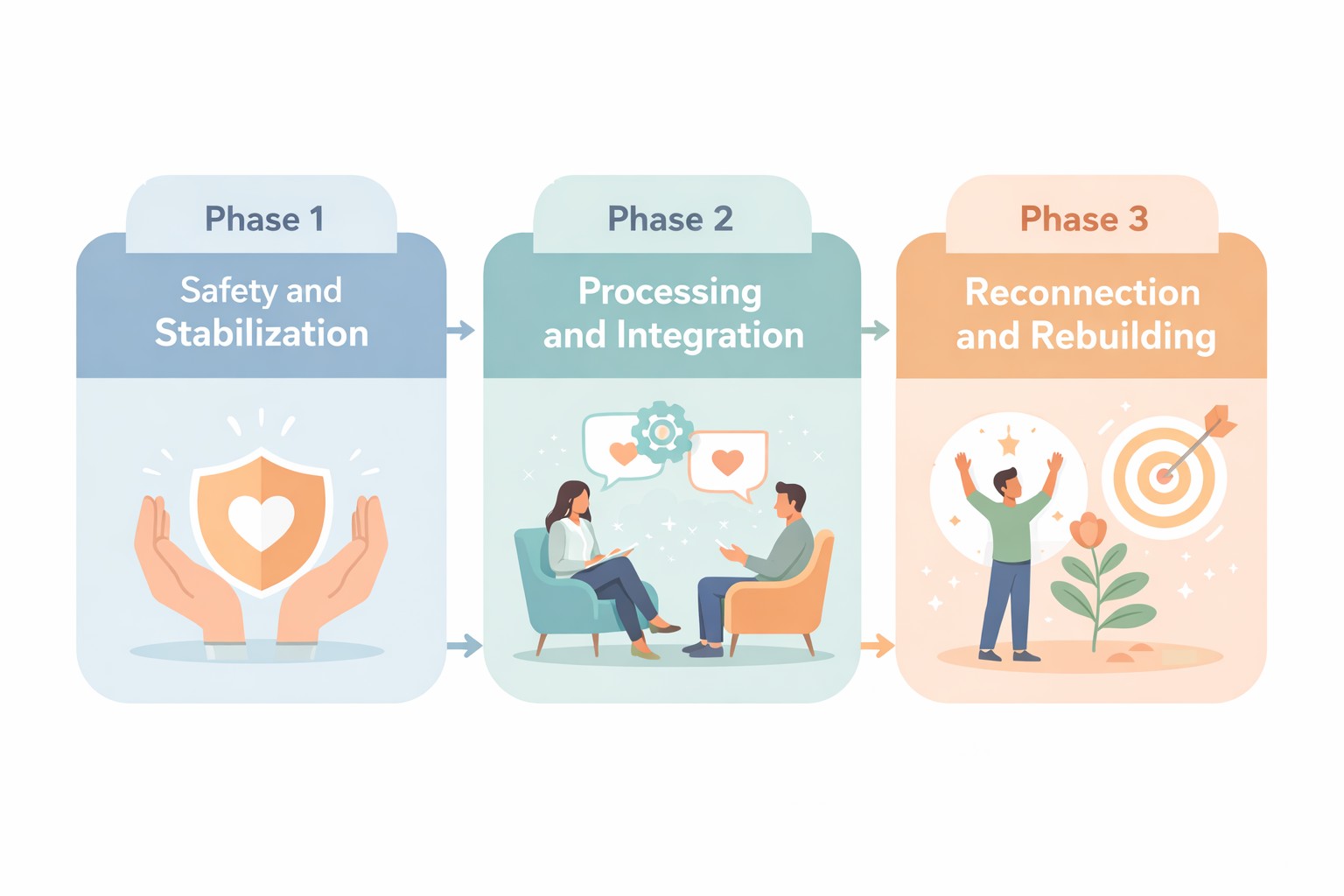
Phase 1: Safety and Stabilization:
This phase focuses on building your internal resources through skills like grounding techniques, emotional regulation strategies, and creating a safety plan. Many people spend several weeks or even months in this phase.
Phase 2: Processing and Integration:
Only after establishing stability do you begin working through traumatic memories using evidence-based modalities like EMDR (Eye Movement Desensitization and Reprocessing), or Cognitive Processing Therapy. This happens at a pace you can tolerate without becoming overwhelmed.
Phase 3: Reconnection and Rebuilding:
As traumatic material becomes less distressing, you work on rebuilding your life, repairing relationships, and integrating your experiences into a coherent narrative that is part of your larger story.
Now the question arises, Which programs best support this phase-based approach?
Unlike standard weekly outpatient therapy, high-intensity treatment requires flexible pacing based on the client’s current functioning and symptom severity. Therapists may increase session frequency during crisis periods when clients show signs of overwhelm, and continuously assess whether the current approach remains appropriate. At our center, we offer intensive outpatient programs that offers several hours of structured programming multiple days per week while you continue living at home.
How Do Specialized Environments Support Complex Recovery?
Where you receive treatment matters almost as much as what treatment you receive. These specialised environments work by reducing barriers to healing and the through:
1. Controlled Clinical Settings
If your home environment is chaotic, it’s extremely difficult to focus on recovery. Residential treatment removes these barriers temporarily, creating a structured environment where your only job is healing. You don’t have to cook, clean, work, or manage daily stressors. It helps you creating the conditions necessary to develop skills you can then apply when you return to your regular environment.
2. Providing Sensory-Sensitive and Trauma-Informed Spaces
Harsh fluorescent lighting, lack of privacy, and sterile environments can actually trigger stress responses in trauma survivors, making it harder to engage in treatment.
High-quality treatment facilities intentionally design spaces to promote calm and safety: natural lighting, comfortable furnishings, access to nature, private rooms, and aesthetics that feel more like a home and support nervous system regulation.
3. Offering Personalization
High-acuity care recognizes that every person’s situation is unique. This might mean adjusting therapy modalities, incorporating holistic practices like yoga or art therapy, modifying communication approaches, or coordinating family involvement.
For individuals with co-occurring disorders, dual diagnosis treatment programs coordinate mental health and substance use interventions simultaneously rather than treating them separately, an approach proven far more effective than sequential treatment.
How Is Progress Measured in Advanced Care Programs?
High-acuity mental health treatment requires more sophisticated progress measurement. That’s why evaluation focuses on how well individuals function, regulate emotions, and maintain stability over time, including:
- Functional recovery tracking, such as the ability to complete daily self-care tasks, engage socially, and use coping skills during periods of distress. These indicators show whether individuals are learning to live well despite ongoing symptom management needs.
- Emotional stabilization monitoring using validated assessment tools that track mood patterns, anxiety levels, frequency of suicidal ideation, and occurrence of crisis episodes.
- Regulation benchmarks, measured by improvements in emotional awareness, distress tolerance without harmful behaviors, effective use of grounding techniques, and the ability to return to baseline after triggering events.
Who Benefits Most From High-Intensity Mental Health Programs?
While high-acuity care serves anyone with severe psychiatric symptoms, certain groups particularly benefit from intensive interventions:
- Complex Trauma Survivors: Individuals with histories of chronic abuse and multiple traumatic events requiring specialized, phased treatment approaches.
- Treatment-Experienced Patients: Those who have completed multiple outpatient therapy attempts or experienced repeated hospitalizations without sustained improvement.
- High-Risk Individuals: People with active suicidal ideation, self-harm behaviors, or severe substance use requiring constant monitoring.
- Those with Severe Functional Impairment: Individuals unable to maintain employment, relationships, or basic self-care due to psychiatric symptoms.
- Co-occurring Disorder Presentations: Patients with multiple intersecting conditions requiring integrated, comprehensive treatment approaches.
How Is High-Acuity Care Different From Visual Acuity?
You might be searching for information about mental health treatment and getting results about eye exams. Let’s clear up the confusion: these terms are completely unrelated despite sharing the word “acuity.”
High visual acuity refers to your eyes’ ability to distinguish fine details, typically measured with an eye chart. A score of 20/20 means normal visual acuity and you can see at 20 feet what a person with normal vision sees at that distance.
In contrast, high acuity in mental health describes the severity and urgency of psychiatric conditions requiring intensive treatment. The word “acuity” simply means “sharpness” or “intensity” in both contexts, but one refers to vision clarity while the other refers to illness severity. They’re entirely separate medical concepts.
Why Do Precision, Privacy, and Time Matter in Complex Mental Health Care?
High-quality high-acuity care is defined by precision, privacy, and time. Advanced programs move beyond generic protocols, where precision ensures that the program responds to the whole clinical picture rather than forcing patients into standardized pathways.
Privacy and time are equally essential, since many individuals delay care due to professional or social concerns, making discreet intake and protected treatment settings critical.
At the same time, complex mental health recovery cannot be rushed as trauma integration often requires weeks or months of consistent care. Programs that allow adequate time, support lasting healing rather than temporary symptom relief.
What Should You Do If Standard Care Isn’t Enough?
Recognizing that standard mental health treatment isn’t providing adequate support is an important first step. If you or someone you care about shows signs of needing high-intensity care, taking action quickly can prevent crisis escalation and create pathways to recovery.
- Begin by seeking a comprehensive mental health evaluation from clinicians, that will examine the complete psychiatric history, current symptom severity, and co-occurring conditions.
- Contact specialized treatment facilities that offer high-acuity programming. Reputable programs will conduct thorough pre-admission screenings to ensure their services match your specific needs.
- Request for confidential evaluation process. These evaluations can often be completed via secure telehealth platforms, allowing you to explore options without public exposure or professional disruption.
Ready to Explore High-Acuity Care Options?
If you or someone you care about is struggling with severe mental health symptoms that haven’t improved with standard treatment, we encourage you to reach out at 516-928-6392. Our clinical team will help you understand your options and determine which level of care best serves your path to stability and wellness.
Contact Legacy Healing today to learn how our specialized mental health programs can support your journey toward recovery. You deserve care that actually meets your needs, and we’re here to provide it.

Dr. Ash Bhatt MD. MRO
Quintuple board-certified physician and certified medical review officer (AAMRO) with 15+ years of experience treating addiction and mental health conditions. Read More…
Table of Contents
Most Insurance Policies
Cover Treatment.
Find out what treatment programs you qualify for in less than 2 minutes.
"*" indicates required fields
Ready to Get Help?
One call can change everything. Our experienced admissions team is here to guide you to the right treatment. All calls are 100% confidential.





